07.25.22
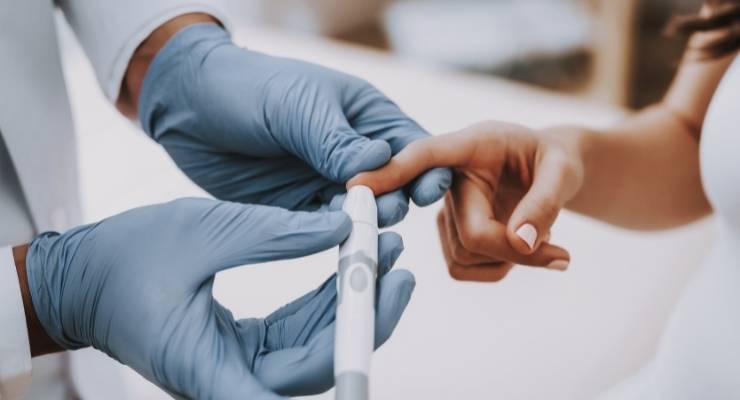
A three-month intervention of folic acid supplementation appeared beneficial to fasting blood glucose, HbA1c, serum insulin, and insulin resistance in a group of 100 patients with type 2 diabetes, according to a study published in Nutrition and Diabetes.
In the present study, the 100 patients were divided into two groups that either received a placebo or folic acid in a 5 mg dose daily for 12 weeks. Folic acid supplementation was linked to a significant decrease in homocysteine and sortilin serum levels (28.2% and 33.7% respectively). Both of these biomarkers are correlated to insulin resistance, dyslipidemia, and poor control of the disease, according to the authors.
After three months of the intervention, the participants who received the supplement saw an 8.7% decrease in fasting blood glucose, a 13.7% decrease in serum insulin, and a 21.7% decrease in measurements of insulin resistance. No significant changes in any of these domains were observed in the group that was given a placebo. Additionally, neither group saw a significant change in lipid profiles after the 12 week intervention.
Several mechanisms have been proposed for the involvement of folic acid in the pathogenesis of insulin resistance and type 2 diabetes, the authors wrote. Hcy, which is reduced by folic acid, may lead to a suppression of glycogen production, they said. Additionally, folic acid has been linked to endothelial dysfunction, which is beneficial to glycometabolism.
“[Folic acid supplementation] could have a possible contribution in the primary prevention of cardiovascular events in diabetic patients,” the authors concluded. “Homocysteine and sortilin could be used as therapeutic targets for T2DM treatment and could aid clinicians for identification of cardiovascular risk in diabetic patients.”
In the present study, the 100 patients were divided into two groups that either received a placebo or folic acid in a 5 mg dose daily for 12 weeks. Folic acid supplementation was linked to a significant decrease in homocysteine and sortilin serum levels (28.2% and 33.7% respectively). Both of these biomarkers are correlated to insulin resistance, dyslipidemia, and poor control of the disease, according to the authors.
After three months of the intervention, the participants who received the supplement saw an 8.7% decrease in fasting blood glucose, a 13.7% decrease in serum insulin, and a 21.7% decrease in measurements of insulin resistance. No significant changes in any of these domains were observed in the group that was given a placebo. Additionally, neither group saw a significant change in lipid profiles after the 12 week intervention.
Several mechanisms have been proposed for the involvement of folic acid in the pathogenesis of insulin resistance and type 2 diabetes, the authors wrote. Hcy, which is reduced by folic acid, may lead to a suppression of glycogen production, they said. Additionally, folic acid has been linked to endothelial dysfunction, which is beneficial to glycometabolism.
“[Folic acid supplementation] could have a possible contribution in the primary prevention of cardiovascular events in diabetic patients,” the authors concluded. “Homocysteine and sortilin could be used as therapeutic targets for T2DM treatment and could aid clinicians for identification of cardiovascular risk in diabetic patients.”